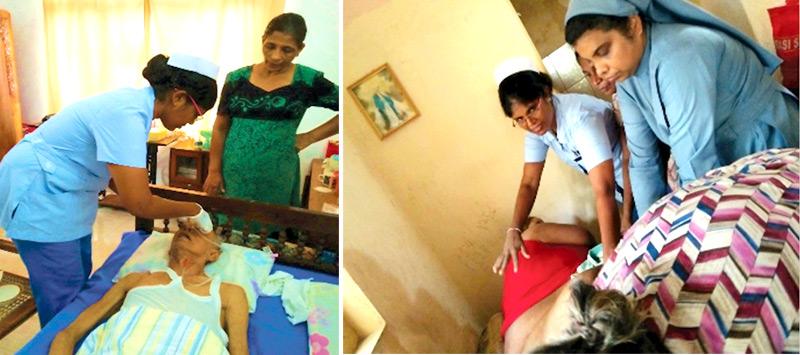
When World Hospice and Palliative Care Day was observed last week (9), it brought together all those directly or indirectly involved in the care of patients with life threatening diseases.
 As this is a subject which is still not well understood by our readers, and is sometimes not accessed due to myths and wrong beliefs, the Sunday Observer spoke to Consultant community Physician, Palliative Care Unit, National Cancer Control Program (NCCP) Ministry of Health, Dr Irosha Nilaweera to explain what it meant, for whom this care was specifically targeted to and why it was introduced in the first place.
As this is a subject which is still not well understood by our readers, and is sometimes not accessed due to myths and wrong beliefs, the Sunday Observer spoke to Consultant community Physician, Palliative Care Unit, National Cancer Control Program (NCCP) Ministry of Health, Dr Irosha Nilaweera to explain what it meant, for whom this care was specifically targeted to and why it was introduced in the first place.
Excerpts
Q: Palliative Care is still not properly understood by most people even those who need it. As a physician dealing with the subject, tell us what is palliative care?
A: Palliative care is caring of patients with life-limiting illnesses, relieving their suffering and supporting them and their families. It provides comfort rather than cure with a multi-disciplinary team approach which aims at not adding days to life but adding a comfortable life to the days.
Q: What is the best way to define it in layman’s language?
A: Let me quote The World Health Organization (WHO)’s definition which sums up the gist of what this health specialty means: The WHO defines palliative care as, “An approach that improves the quality of life of patients and their families facing the problems associated with life threatening illness, through the prevention and relief of suffering by means of early identification and impeccable assessment and treatment of pain and other problems, physical, psychosocial and spiritual”.
Q: Two concepts of World Hospice and Palliative Care are celebrated on the same day. Why?
A: World Hospice and Palliative Care Day is for action to support and to improve awareness on palliative care and hospice around the world. It takes place on the second Saturday of October every year. Palliative care got its start as hospice care, often delivered by caregivers at religious institutions. Dame Cicely Saunders, a British physician, founded the first formal hospice in 1948, specifically to care for patients with terminal illnesses.
Q: Your theme each year is different. What is it this year? And what is its significance?
A: This year (9), the theme is, “Leave no one behind – equity in access to palliative care”, showing that palliative care needs to be provided in accordance with the principles of universal health coverage, namely, that all patients with life threatening diseases should have access to palliative care according to their need, irrespective of the illness or its stage and other characteristics of the patient such as age, sex, ethnicity, religion, or the income status.
Q: Are palliative care and end of life care the same?
A: Palliative care is about living as well as dying. There is a misconception that palliative care is only for caring someone in the last few days of his life. Palliative care is about relieving suffering and improving quality of life right from the time when a person is diagnosed that he has a life-threatening illness.
The aim of palliative care is not to lengthen – or shorten – life but to improve quality of life so that the time remaining, be it days, or months, or years, can be as peaceful and fruitful as possible. To quote Ruth Wooldridge (1988) “Put life into their days, not just days into their life”.
Q: Where can end of life support be given?
A: End of life care is support for a patient who is in last months of his life. It should be provided according to the patient’s wishes and preferences. It can be provided at home, hospice, hospital, according to the patient’s needs and preferences. It should help the patient die with dignity and peacefully. The support should also be provided to family members, caregivers and others close to the patient during the period.
Q: Why do we need to add this new specialty to our already overloaded but efficient health care system? Isn’t it a waste of government funds and resources?
A: At present, most of the health care services we have are for treatment and prevention of diseases. However, with epidemiological and demographic transition, it has been found that there is a huge need that is not being met for the ongoing care for those who do not get better and are with terminal illnesses.
It is estimated that worldwide around 40 million people require palliative care each year; 78 percent of them people live in low- and middle-income countries. Worldwide, only about 14 percent of the people who need palliative care receive it.
As for Sri Lanka, the need of palliative care in Sri Lanka continues to grow due to increasing prevalence of non-communicable diseases and ageing population. Data shows that about 75 percent deaths occurred due to chronic non-communicable diseases.
Q: Does palliative care have an age limit? Does it, for example, include children with life threatening illnesses as well?
A: Palliative care is for anyone with a life limiting illness – e. g: in hospital or at home, child or adult, young or old. Palliative care can help patients with many life threatening illnesses: e. g: cancer, heart failure, end-stage lung disease, renal failure, liver failure, progressive neurological illness, dementia, end stage diabetes and other life-limiting illnesses.
Q: What is it that makes palliative care different from any other care?
A: Usually, health care tends to focus on physical problems – diseases and treatments. However, palliative care recognises that patients much more than just a body – mind, spirit and emotions are also parts of the person, as are the families and communities to which he belongs.
So the problems experiencing a sick person and his family are not just physical; there may be psychological, social and spiritual issues which are just as important as the illness itself. Sometimes a problem in one domain may worsen others, e.g: pain is often worse when person is anxious or depressed.
It is only when we address all these issues that we are helping the whole person. This is called holistic care.
Q: What is holistic care?
A: The holistic approach addresses problems in four domains:
Physical – symptoms (complaints), e. g. pain, breathlessness, tiredness and vomiting.
Psychological – worries, fears, sadness, anger and suicidal ideations.
Social – needs of the family, needs of children, issues related to work, housing, finance and relationships.
Spiritual – questions of the meaning of life and death, the need to be at peace.
Q: Is palliative care a substitute for other care programs you already have?
A: Palliative care works alongside and within other programs. It does not replace other forms of care. It can be integrated into existing care and should be a part of the care given to everyone with a life-limiting illness. At the time when someone finds out that his disease cannot be cured, he may be active, busy with work and family life, and may be on treatment such as chemotherapy.
Palliative care should begin alongside with other treatments, helping with difficult symptoms, and giving emotional and spiritual support to the patient and the family. As time goes by, with the progression of the disease, needs will be changed. For example, they may need more symptom control.
Other treatments may be stopped if they are no longer helping and holistic palliative care is what will help the most. Even after death, palliative care can be continued by giving bereavement support to family and loved ones of the patient.
Q: Who comprises the team that provides palliative care?
A: A multi-disciplinary team of palliative care includes many members: health as well as non-health.
Consultants
Doctors
Nurses
Psychologists
Counsellors
Physiotherapists
Occupational therapists
Nutritionists
Social workers
• Other government officers
Religious leaders
Volunteers
Q: Where is palliative care available?
A: Palliative care services are available in three settings. 3 ‘H’ –
(1) Hospital
(2) Hospice
(3) Home
Hospital Care
Specialist care is provided at major hospitals: treating specialist unit or through multi-disciplinary approach, e. g: Palliative Care Consult Service at Apeksha Hospital, Maharagama. The first palliative care centre with inward facilities attached to a state hospital was established at the Teaching Hospital, Karapitiya in 2020. At the Primary Healthcare level, services are provided by health care teams at primary healthcare hospitals and General Practitioners.
Hospice care
Hospice is a dedicated institute where supportive care is provided for the patients’ emotional, social, and spiritual needs in addition to the care for the remaining physical symptoms following active disease specific treatment by an inter-disciplinary team. There are seven hospices in Sri Lanka. These hospice services are provided by Non-Governmental Organisations. The services are free of charge.
Community care
The contribution of community palliative care services in coordination with primary and specialist care service providers is essential as the majority of palliative patients live the balance period of their life at their home. It should be provided with a multi-disciplinary approach: e.g. officials attached to the Divisional Secretariat Office, community-based organisations and religious leaders.
Care at home
A caregiver is a person who is caring for a palliative patient and helps to improve the patient’s wellbeing. The caregiver can be a paid carer, a family member or a volunteer carer. Caring for a palliative patient is a demanding work, and caregiving without adequate knowledge, skills, support and self-care can harm the patient. A caregiver of a palliative patient should have knowledge /skills on following areas:
Physical, psychosocial and spiritual status of the patient.
How to communicate to the patient.
Basics of nursing care.
How to administer medicines prescribed.
When and where to seek help, support for the patient and also oneself.
Home based care is supported by trained community healthcare workers or volunteers. The Public Health Nursing Officer (PHNO) who is attached to primary health care hospitals, is responsible for home visits and assesses palliative care needs at the home setting. In addition, selected hospitals have health care teams providing home based care e.g. District General Hospital Monaragala, District General Hospital – Nuwaraeliya, Base Hospital, Thelipallai, and Teaching Hospital Ratnapura.
Q: Do you see the need for palliative care increasing with Sri Lanka’s rapidly aging population?
A: The need for palliative care in Sri Lanka will continue to grow as a result of the ageing of populations and the rising burden of non-communicable diseases and some communicable diseases. However, palliative care is still an evolving area and has a long way to go in Sri Lanka. With the increase in the establishment of services, the quality of life of those suffering from life threatening illnesses and their families, will be better in the future than at present.
