Due to interventions by the Anti Leprosy Campaign and the Health Ministry the disease has declined drastically. The key to beat Leprosy is educating society on all aspects of the disease and the cooperation of the public, says Consultant Dermatologist, Anti Leprosy Campaign , Colombo Municipal Council, and National Hospital Colombo, Dr Indira Kahawita. With her hands on experience she discusses the main issues faced by patients, highlighting that changing public attitude to patients and encouraging them to seek treatment readily available at the Central Leprosy Clinic at the National Hospital Colombo is the need of the hour in an interview with the Sunday Observer.
Excerpts
 Q. When Leprosy Day was observed recently (January 31) what was the theme that was highlighted and its significance?
Q. When Leprosy Day was observed recently (January 31) what was the theme that was highlighted and its significance?
A. This year’s theme is “Beat Leprosy”- its significance being our need to defeat the disease in every aspect, be it clinical, social or psychological.
Q. As many still don’t know what exactly leprosy is, tell us what this disease is and the signs to look for.
A. Leprosy is a bacterial infection affecting the skin and the nerves. The bacterium is slow growing and takes a long time to manifest clinically after someone acquires the infection. It may present as skin patches with sensory loss and /or neurological manifestations. It is the neurological problems that lead to most of the consequences due to leprosy.
Q. What causes it?
A. The bacterium causing leprosy is called Mycobacterium leprae. It is a slow growing bacterium which survives inside cells. The bacterium mainly affects humans. The only other potential hosts being nine banded Armadillo and mice
Q. Is it transmissible? How?
A. Through respiratory droplets. A person with the infectious forms of leprosy can secrete the organism in the droplets when breathing, talking or sneezing. It is usually not transmitted by touch. Therefore, you need not fear to touch someone with leprosy.
Q. Can anyone get leprosy? Who are those most at risk of getting it?
A. Persons of any age or any social status can be susceptible to leprosy. Even though it is seen more commonly in persons with low socio-economic status, the real reason may be overcrowding and easy transmission rather than the social status.
Q. Can one inherit leprosy?
A. Leprosy is not an inherited disease. But persons living within the same household with someone having the infectious forms of leprosy are more susceptible to catch the infection. It is the prolonged close contact (breathing the same air) that causes the susceptibility, not the heredity.
Q. What about infants and very young children?
A. Infants and very young children may also be infected but the disease is not common in infancy, probably due to the long incubation period. On the other hand approximately 10 percent of our annual case load comprises children below 15 years.
Q. What are the first signs of leprosy?
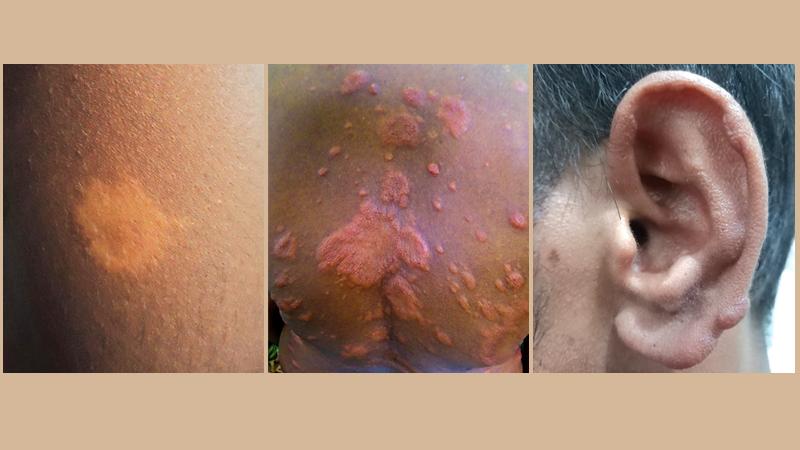
A. The commonest sign of leprosy is one or a few pale skin patches with impairment or loss of sensation with the patch. During the early infection these symptoms and a thickened peripheral nerve may be the only signs.
Q. Can a person with these symptoms transmit the infection to others?
A. No. A person with such lesions cannot transmit the disease to others.
Q. Symptoms as it advances?
A. In the more advanced disease there may be many skin lesions without sensory impairment and more nerves may be affected. Such lesions may easily be misdiagnosed as other skin diseases such as aluhang. The more advanced, infectious form of the disease may also show change in facial appearance, e.g. the earlobes and eyebrows may thicken with the whole face being puffed up. By this time they may have nasal stuffiness indicating involvement of the mucosal surfaces. Such patients may also have numbness of hands and feet.
These patients are capable of transmitting the infection to others. It also affects the eyes. In some patients weakness of nerves supplying the facial muscles may lead to incomplete closure of eyes, dryness due to exposure and blindness. In some patients the entire eye may be affected with painful red eyes and difficulty in facing a light (photophobia). Fortunately, blindness due to leprosy is rare in Sri Lanka.
Q. Treatment- How do you treat them?
A. Treatment is with a combination of drugs called “Multi Drug Therapy (MDT)”. The drugs are provided free of charge by the WHO (World Health Organization). The less severe form is treated for six months. Infectious forms need treatment for a minimum of 12 months.
Q. Is there a vaccine to prevent leprosy?
A. There is no vaccine for leprosy. Vaccine trials are being conducted in India, but we cannot expect that the vaccine will be able to stop transmission. Like the vaccines for tuberculosis they may only reduce the severity of the infection.
Q. Is the treatment the same for infants, the young and the older victims?
A. The drugs are the same. The doses vary according to age and body weight. There are two types of blister packs for adults and children between 10 and 14 years. For younger children the doses are adjusted according to body weight.
Q. Do you have any new data on leprosy patients in Sri Lanka?
A. According to data from the Anti Leprosy Campaign Sri Lanka, the number of new cases reported each year in the country has remained constant, around 2,000 since year 2000. But we have seen a slight decline in the number of new cases during the past few years. According to the Weekly Epidemiological Record published by the WHO in 2020, the number of new cases reported in Sri Lanka in 2019 is 1,658, of which 176 (10.61%) were children. There were 91 patients (5.48%) with visible disability (neurological deficit in hands/ feet or eye involvement) at the time of diagnosis.
Q. Do you think actual numbers could be higher due to their being unreported?
A. All diagnosed cases are reported so the problem of under reporting at health care institution level does not occur. Our main concern is the diagnosis being missed, either due to patients not seeking treatment or doctors not suspecting leprosy.
Q. Who can identify them?
A. Any health care worker aware of the major signs and symptoms should be able to suspect leprosy. Confirmation is usually done at skin clinics country wide.
Q. How is this done?
A. In most instances the diagnosis is done by a thorough examination of the patient but sometimes investigations like a skin smear (examination of a sample of tissue fluid under the microscope) or a skin biopsy (to look at the changes in the skin due to leprosy) may be necessary in doubtful cases
Q. Can it be cured with early detection?
A. Leprosy can be cured without disability if detected early. Our concern is that patients disregard the early symptoms and seek treatment when the nerves have been severely affected. In such instances the nerve damage may persist despite treatment. In Sri Lanka the percentage of patients who have profound nerve damage at diagnosis is around five to seven percent.
Q. Once treated and cured can a patient get re –infected?
A. A small number of people present with features of leprosy after successfully completing a course of treatment. But this is rare.
Q. When is someone considered non-infectious to others after starting treatment?
A. The drugs used to treat leprosy are strong antibiotics, hence, they can kill a large number of bacilli within a short period. We can safely assume a patient to be non-infectious one month after starting appropriate treatment.
Q. What happens to a victim if the condition is untreated for some reason?
A. If the disease is left untreated the nerve damage may continue. The patient may end up with permanent neurological problems like weakness of muscles (claw hand or foot drop) or permanent sensory loss in hands and feet leading to subsequent ulceration. This sensory loss and ulceration may lead to shortening of digits in neglected cases. It was this deformity that was referred to as ‘dropping off of fingers’ by many lay persons. But in effect this is not different from the ulceration of digits that occurs in those with Diabetic neuropathy.
Q. Main obstacles that prevent patients from seeking early treatment? Is it stigma?
A. In my opinion stigma is not the main cause why patients do not seek treatment. It is not being aware of leprosy as a disease entity prevalent in Sri Lanka.
Q. What are the most common myths in Sri Lanka and where are such myths prevalent?
A. One common myth is the ‘dropping digits’. Another common myth is about leprosy and heredity. No one can pass the infection genetically to their offspring even though they may get infected due to close contact within the household.
Q. How has your Association met this challenge?
A. More than myths what we have had to address over time is the society’s reactions to persons affected with leprosy. When someone is diagnosed with leprosy there is a tendency for work colleagues to keep away from them due to various misconceptions about its infectivity.
Q. Is public awareness of leprosy, including the medical and social implications of the disease and the rights of persons affected, your current focus?
A. Yes, it is the current need. The public needs to know the signs and symptoms of leprosy to ensure that they seek treatment promptly. In addition, society must be aware that leprosy is not different from any other skin disease. This will ensure equal status to patients affected with leprosy, without discrimination or stigma.
Q. In our technologically advancing nation how do you see the future for leprosy patients in Sri Lanka?
A.The prognosis for patients with leprosy is good. The vast majority will get cured without any disability or lasting signs of the infection, without help from high tech methods for diagnosis.
It is the timely intervention, and the compliance of the patients for a fairly long course of treatment and supportive treatments like physiotherapy that determines the success of treatment.
Q. Gaps you’d like to fill in ensuring optimum benefits in care for leprosy patients?
A. The need of the hour is awareness on the real facts about leprosy. In addition, we need a change in the public’s attitude towards diseases as a whole.
Q. Your message to the general public?
A. Beating leprosy requires team effort. We need public support in detecting cases, providing care and ensuring a fruitful life for persons affected with leprosy so that together we can beat leprosy.
Q. What is your Message to persons with suspected symptoms reluctant to seek treatment?
A. Leprosy is curable especially if diagnosed and treated early. So don’t hesitate to seek treatment if you suspect you have leprosy. You can be treated at the nearest skin clinic. In addition, the Central Leprosy Clinic at the National Hospital of Sri Lanka functions as a walk in clinic, so that you may just visit us and discuss your fears.
