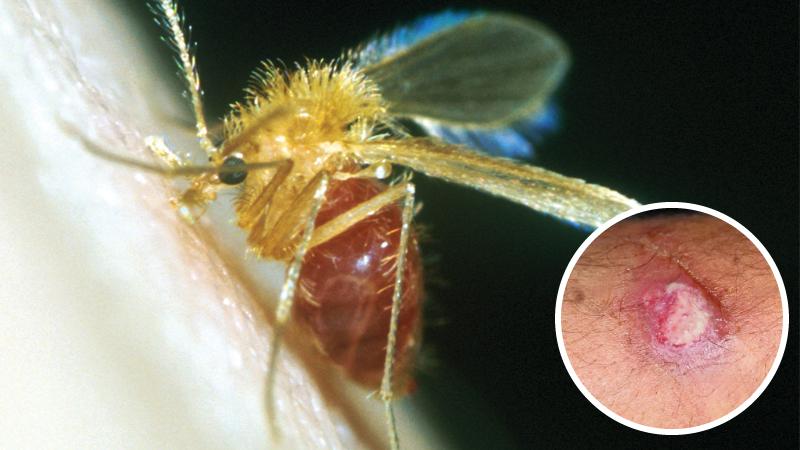
It is a disease caused by a tiny sandfly – so tiny that it is not visible to the naked eye. Yet victims exposed to it can suffer from lifelong scars and ugly sores if they don’t seek early treatment. The good news is that it is completely curable if patients bitten by the insect seek early treatment.
The Sunday Observer spoke to Consultant Epidemiologist, Epidemiology Unit, Ministry of Health and Indigenous Medical Services, Dr. Manjula Kariyawasam to find out more about this little known endemic disease and if the current climatic changes had any bearing on the recent spate in this zoonotic disease.
Excerpts…
Q. Several cases of Leishmaniasis have been recently reported in different parts of the Island. Not many people seem to know much about the disease which if neglected could lead to more complications. Explain what Leishmaniasis is.
 Dr. Manjula Kariyawasam |
A. Leishmaniasis is a vector-borne parasitic disease. This parasite is named Leishmania. It transmits through the bite of an infected female sandfly. Cutaneous leishmaniasis (CL) is the commonest form which causes skin lesions, mainly ulcers, on exposed parts of the body, leaving life-long scars and disability which may cause a stigma.
Q. What are the early signs/symptoms of this disease?
A. Let’s limit to the Cutaneous Leishmaniasis as it is the commonest in Sri Lanka. Initially it starts as a skin lesion with the appearance of a small papule. Usually it occurs one to two weeks to several months after the sandfly bite. The papular lesion could develop into a nodular lesion that may enlarge and become a chronic ulcer. These lesions usually develop in exposed areas of the body such as the face, neck, arms and legs as single or multiple lesions. This is because the sandfly bite cannot pierce through the clothes. Lesions are usually painless and non-itchy.
Q.. For how long do they last? Does it depend on the individual case?
A. If the infected person has not sought treatment it could last many months. Very few may heal spontaneously over months to years, leaving an ugly scar.
Q. If a person has a pre-existing health issue like diabetes can this prevent or prolong the duration of recovery?
A. Obviously, due to the pathophysiological changes of chronic diabetics, it could delay the wound healing.
Q. Is it curable?
A. Yes, it’s a completely curable disease.
Q. Do the rashes and other complications go away after a while or do they remain?
A. Skin lesions will resolve with the treatment. The earlier the treatment, the earlier and better the cure.
Q. Is it treatable? How do you treat it? With western drugs or local applications?
A. Yes, it is treatable. The most commonly used method is called “cryotherapy” where the Dermatologists apply liquid nitrogen using a special device. In certain instances, Dermatologists may give drugs via injections mainly. The treatment is offered in outpatient clinics in hospitals where a Consultant Dermatologist is available, which means there is no need to get admitted to receive treatment.
Q. How effective are these treatment methods?
A. Most are very effective.
Q.Is the treatment tailor-made for each patient?
A. Yes. We follow the clinical guidelines and protocols to treat these patients. The treatment modality depends on various factors such as the site of the lesion, number of lesions, or body weight of the patient.
Q. What about pregnant women? Can they pass it on to their unborn child?
A. As the parasite is confined to the skin lesion, the disease will not cause any harm to the foetus of the pregnant mother infected with the disease.
Q. Babies and toddlers – are they at risk?
A. They also have a similar risk as the others.
Q. Leishmaniasis is also called sandfly disease. Why?
A. This is due to the incriminated vector, the sandfly. It is also locally known as weli messa or Ho Haputuwa.
Q.Does the vector belong to the same family of mosquitoes that cause dengue and malaria?
A. This vector does not belong to the mosquito family. It’s a fly and not a mosquito. Mosquitoes and flies belong to the same Phylum called Arthropoda, but to two different families. Flies are in the Phlebotomidae family while the mosquitoes belong to the Culicidae family
Q. Can you describe the sandfly?
A. Sandflies are small insects with two to three millimetres in body length. Body colour varies from light brown to black with hairy appearance, large black eyes and long, stilt-like legs. They keep their wings in a characteristic V shape while resting. Sandflies are weak and silent flyers with hopping movements.
Even though female and male sandflies feed on plant juices, females take blood meal to mature the eggs. The common resting sites of adult sandflies are cracks and holes in rocks, caves, and rodent burrows, cool, dark and humid corners of animal shelters or human dwellings in peri-domestic settings.
Common breeding places include bark and buttress roots in old trees, animal shelters, cracks and holes in floors and walls, household garbage dumps which are rich in moisture and humus.
Q. When was it first reported in Sri Lanka?
A. In the 1990s. It has been included in the list of notifiable diseases since 2008.
Q. Does that mean it is an infectious disease?
A. Yes, it’s an infectious disease. Like malaria, it’s caused by a parasite known as Leishmania. It cannot transmit directly from human to human or animal to human. Vector is the one who transmits the disease.
Q. What is the role of the Epidemiology Unit in identifying the disease?
A. The Epidemiology Unit of the Ministry of Health is the national focal point for control and prevention of Leishmaniasis in Sri Lanka.
As one of the notifiable diseases in the country, it is mandatory to notify any suspected case of leishmaniasis to the Medical Officer of Health by the treating physician.
Q. According to recent studies by the Epidemiology Unit in what parts of the island have you found the highest number of cases district wise and zone wise. Is climate change a contributory factor?
A. The first local case of cutaneous Leishmaniasis was reported in the Ambalantota Medical Officer of Health area in the Hambantota District in 1992. Since then the disease has spread to many parts of the country and is now established as an endemic disease.
Nearly 4,000 cases have been reported to the Epidemiology Unit during 2019 alone. Five districts namely, Anuradhapura, Polonnaruwa, Kurunegala, Hambantota and Matara contribute to approximately 90% of the annual caseload. In addition, Matale, Kegalle and Gampaha have shown an increasing number of cases during the past two years.
To answer your second question, although a majority of the cases are reported in the dry zone, some districts in the intermediate and wet zone are also reporting cases.
Hence, we could not come to a conclusion of any direct climatic conditions related to the disease. There are multiple factors other than climate which facilitate the disease transmission.
Most of the factors favourable for the vector breeding such as rich vegetation and wet alluvial soil could facilitate the transmission of the disease.
Q. Are villages close to forests more vulnerable?
A. This disease is a zoonotic disease. That means the disease can transmit from animal to human through sandflies. Unlike other countries where the disease is endemic and there are several animal reservoirs, according to the available limited scientific evidence such a reservoir host has not been identified in Sri Lanka.
However, the human is a reservoir for transmitting the disease. That means the infected individuals act as a reservoir for the parasite to transmit to another human through the vector.
Q. Can other animals such as rats, bandicoots, monkeys, dogs, pigs transmit the disease to humans?
A. Yes, different reservoir animals have been identified in the endemic countries. including rodents and other mammals. However, to date, the available evidence does not prove or disprove the availability of such reservoir animals in Sri Lanka.
Q. Are there specific types of Leishmaniasis. What are the common types in Sri Lanka?
A. Three main clinical manifestations of leishmaniasis are present namely, Visceral Leishmaniasis (VL), Muco-Cutaneous Leishmaniasis (MCL) and Cutaneous Leishmaniasis (CL). CL is the predominant type reported in Sri Lanka. However, a few sporadic cases of VL have also been reported mainly among overseas exposures.
Q. Is there a new emerging trend in the disease where sandflies are now being observed in new areas?
A. There is written evidence of the presence of sandflies since 1940, and that sandflies are present in most parts of the country.
Therefore, due to the presence of the parasite in the infected persons and the availability of the vector, the disease can spread easily to new frontiers which are adjacent to endemic localities.
Q.Your message to those living in high risk areas?
A. To minimise indoor resting of sandflies, keep the houses clean regularly, allow in sunlight and facilitate air circulation in the premises.
Old buildings, animal shelters and huts made with mud thatched walls with cracks and holes provide a conducive environment as breeding sites to sandflies. Plastering the walls and floors with cracks and holes evenly with a suitable plastering material will avoid breeding sites.
Breeding sites and outdoor resting places of the sandfly can be eliminated by keeping the outdoor environment clean. Avoid unnecessary vegetation, allow sunlight to fall and provide adequate air movement by removing unnecessary items such as shady tree branches, broken parts/ debris near houses.
Avoid garbage dumping and decaying items near houses and control rodent habitats. Avoid growing shady trees, bushes close to animal shelters. Clean the animal shelters by removing animal waste regularly and keeping them dry.
The sandfly is mainly active from dusk to dawn. To prevent/minimise vector contact, outdoor activities should be avoided as much as possible, especially outdoor sleeping, during this period. Protective clothing should be worn (long sleeved shirts, ankle length pants) that cover the whole body when working outdoors, in animal shelters and during play outdoor.
Insect repellent should be applied to uncovered skin and under the sleeves and pant legs. Re application of repellants need to be done as they are effective only for 4-6 hours.
Q. What about bed nets?
A. Bed nets impregnated with pyrethroid-containing insecticides should be used if available. Untreated bed nets do not prevent sandfly entry due to the small size of the insects.
