
The neonatal period is the most vulnerable period for child survival. Yet although neonatal mortality has declined in Sri Lanka it continues to be a health issue that worries the medical community.
Here Consultant Neonatologist University Neonatal unit , De Soysa Hospital for Women, Colombo, and Senior Lecturer, Dept of Paediatrics, University of Colombo, Dr. Nishani Lucas discusses skin to skin contact and early breastfeeding as two of the most powerful interventional tools among others, to help premature babies develop their full potential.
 Following are excerpts from her interview with the Sunday Observer.
Following are excerpts from her interview with the Sunday Observer.
Q: Three days ago we observed World Prematurity Day. Why is a special day being dedicated to observe this day worldwide amid other health issues faced by newborn babies?
A. World Prematurity Day is observed to raise awareness about babies who are born too soon and the impact it can have on their families. Every year 15 million babies are born preterm, accounting for one in ten babies born worldwide (WHO, 2018).
Q: What is the global theme for this year’s Prematurity Day and its relevance in changing the future for a better one for children born prematurely?
A. The theme for this year’s World Prematurity Day is “A parent’s embrace: a powerful therapy. Enable skin-to-skin contact from the moment of birth.” This is to raise awareness about Kangaroo Mother Care (KMC) where parents play a central role in providing prolonged skin-to-skin contact to their preterm baby. KMC improves the heat regulation, helps to establish breastfeeding, improves immunity, improves bonding, neurodevelopmental outcomes and reduces neonatal mortality by about 40 percent (WHO, 2020).
Q: Although Prematurity Day has been observed globally since 2011, many readers still do not understand what prematurity is. How do you define a Preterm or Premature infant.?
A. Usually, a pregnancy lasts for 37-40 weeks from the time menstruation ceases (period of amenorrhea). This is known as ‘term’ gestation which is required for the baby’s organs to mature and adapt to survive independently after birth. However, some babies are born before 37 weeks due to the mother going into preterm labour or having to terminate the pregnancy to save the life of the mother, in which case we say that the baby is born preterm (before reaching term gestation) or prematurely (before reaching full maturity).
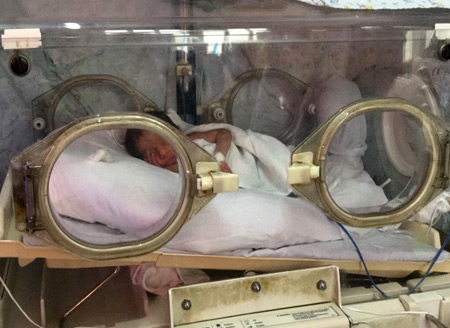 Q: Is it correct that preterm births are an important cause for neonatal deaths? Have you any updates on the latest figures globally and in Sri Lanka?
Q: Is it correct that preterm births are an important cause for neonatal deaths? Have you any updates on the latest figures globally and in Sri Lanka?
A. Yes, it is. About one million children die every year due to the complications of Prematurity worldwide and is the leading cause for deaths under 5 years of age worldwide (WHO, 2018). In Sri Lanka, deaths due to prematurity accounted for just over 50 percent of all neonatal deaths from 2017-2019.
Q: Going by these figures, how would you rank Sri Lanka in the percentage of neonatal deaths?
A. Sri Lanka is far ahead of its neighbouring South Asian countries and is on par with high income countries in terms of neonatal mortality which was 5.7 – 6.1 deaths per 1000 live births as per 2017-2019.
Q: Does the weight of a pre-term baby matter? What is the average weight of pre-term infant and a baby born after full completion of pregnancy?
A. Yes it does. If a baby has grown appropriate for its period of gestation, complications are only limited to prematurity. However if the baby is small for the gestational age there will be complications of prematurity in addition to complications of growth restriction. It is difficult to give an average weight as it depends on the gestation. The lowest survival weight is 500g below which survival is extremely unlikely. The average weight of a full term baby is around 2.8kg in Sri Lanka.
Q: Congenital Diseases are also on the increase in Sri Lanka. Is this an outcome of preterm birth?
A. No, it is not associated with preterm birth. However, it is an independent problem which is almost an equal contributor to neonatal deaths. It has been the commonest cause for infant deaths over the past few years,
Q: Recent studies have reported that many survivors of preterm birth face a lifetime of disability, including learning disabilities and visual and hearing problems. Do you agree?
A. No. I do not agree. The rate of intact survival has increased, and disability is much less than it used to be due to many reasons: better care and facilities being developed with increasing awareness and training, availability of surfactant, parenteral nutrition, non-invasive ventilation, provision of breast milk, developmental care, neurodevelopmental assessment and early stimulation, early skin to skin care, discharge planning. Good care will ensure intact survival with normal neurodevelopment.
 Q: I read that there is new scientific evidence showing that such children also have higher risk of blindness due to retinopathy. Is this correct?
Q: I read that there is new scientific evidence showing that such children also have higher risk of blindness due to retinopathy. Is this correct?
A. Again, this is not new. Screening for retinopathy of prematurity has been done for quite a while with the help of the ophthalmologists, where every preterm baby les than 34 weeks is screened at 21 days even if they are still in the neonatal unit.
If the retinopathy is detected and treated early, blindness does not occur, so limiting the use of oxygen (oxygen increases the risk of retinopathy) while replacing oxygen with non-invasive ventilation machines, in addition to increased surveillance has resulted in minimizing/eliminating the risk of blindness. None of the babies born in our unit have had blindness over the last 10 years.
Q: In addition they have a higher risk of bone disease due to mineral loss. True or false?
A. True
Q: Does this mean this could lead to early fractures and ligament problems and result in arthritis and osteoporosis?
A. Yes there could be fractures, if this condition is undetected. Osteopenia of prematurity is due to immaturity in the preterm kidneys leading to loss of minerals, especially calcium and phosphate. We screen for this condition by 14 days and provide calcium and phosphate supplements, after which we keep monitoring the baby until 40 weeks gestation / or 2kg at minimum.
Q: What are the chances of such children growing up to live as normal people?
A. If the baby does not have any birth defects or get a bloodstream infection or an intracranial bleed there is a good chance, the baby will lead a normal life. At present our intact survival (otherwise normal) rates are around 40-50 percent for 25-26 weeks and around 70-80 percent for 27-28 weeks gestation if delivered in a level III Neonatal Unit, under the care of Neonatologist (Provincial level Teaching Hospitals / Specialised Maternity Hospitals).
Q: We are still in the midst of Covid 19 and new disease outbreaks . As you just said most preterm babies have low immunity levels , are they at higher risk of these infections than children born at full term maturity?
A. Yes, they are.
Q: How do you protect such children from being exposed to these infections?
A. Ensure they receive breastmilk and skin to skin care which improves their immunity.
Ensure minimal handling, hand washing and that everyone entering the neonatal unit wears a face mask.
Q: The current thinking is that children born too soon can survive if they receive the right care in the right place. Do you agree?
A. Yes, most definitely. Transferring a preterm baby after birth increases the risk of intracranial haemorrhage as well as hypothermia, each of which are independent risk factors for prognosis. Therefore, babies less than 32 weeks gestation and less than 1500 g should be transferred before delivery in a level III neonatal unit.
Q: So what is the right time?
A. Before being born
Q: Is the right kind of care a team effort? Who comprises this team ?
A. It is a team effort by doctors, nurses, physiotherapists, speech therapists and parents.
Q: The value of natural nutrients contained in breast milk is a well known fact. How early can a mother breast feed her preterm baby if he or she is in an incubator?
A. As soon as they are born. Breast milk provides all nutrients required by the baby and enhances immunity and improves brain growth.
Q: Should a mother with Covid be encouraged to breastfeed her pre- term baby ?
A. Yes. Breastfeeding will protect the baby from Covid, as it transfers antibodies made by the mother to fight Covid. Therefore, it is vital that breastfeeding is continued. If the baby is still in the neonatal unit, the mother can send expressed breast milk which can be given to the baby. Mother can resume visiting the baby after 14 days. This is due to this mother infecting the staff, other mothers etc. If both baby and mother are together, when the mother is detected to be positive, they should not be separated.
Q: Babies of infected mothers- how are they protected against infection while being breastfed?
A. The Mother is asked to wash her hands and wear a mask when handling the baby. This is because Covid is spread through droplets. Spread via breast milk has not been documented. Breast milk is protective against Covid, as it transfers antibodies produced by the mother against Covid to the baby, thereby minimizing the risk of the baby getting Covid.
Q: Does this require a hospital setting?
A. Not unless the mother or baby is having complications due to Covid. They can be discharged home, where they should self-isolate for 14 days. It is important that mother and baby should not be separated.
Q: Briefly tell us what remedial measures have Sri Lankan paediatricians and neonatologists taken to promote the health and survival of children born too soon during its period of existence?
A. Sri Lankan paediatricians and neonatologists have made an immense contribution to promote the survival of preterm babies. They started a subspeciality in Neonatology in 2006, drew up guidelines, protocols and standards, trained all categories of staff, started getting down surfactant to help the baby cope with immature lungs. They also changed ventilation from invasive to non-invasive form to more gentler forms such as continuous positive airway pressure to minimize the harm during ventilation.
We also started parenteral nutrition (intravenous amino acids and lipids), promoted own mother’s breast milk for preterm babies (either through a tube or cup, until baby can suckle), introduced developmental care to control sound, light and make nests for positioning, promoted kangaroo mother care.
We introduced eye screening for retinopathy of prematurity while in the neonatal unit along with the consultant ophthalmologists, discharge planning, training parents resuscitation and how to handle the baby before going home, neurological examination and arranging early intervention, following these babies up for at least 2 years.
Parents are also updated and counselled by the Neonatal team including all doctors and nurses. In addition, if they are noted to need more support, the help of professional counsellors and the psychiatry team is enlisted.
Q: Gaps you wish to see filled in optimal delivery of care for premature children?
A. As more and more preterm babies survive, more and more NICU beds will be required. At present we see babies born as early as 25 weeks and as light as 500g having intact survival with good neurological outcomes. Smaller size vials of intravenous fluids and medication would minimise wastage by using larger dose vials, as they need to be discarded in 24 hours or some are single use.
Q: Your message for parents of premature babies out there ?
A. Your preterm baby is fragile. Take very good care of your baby, especially during the first 2 years of life. Ensure you breastfeed your baby from the first day, that increases the immunity, protects against non-communicable disease and improves neurodevelopment.
Spend time with your baby, talk to him/her, give skin to skin care. Minimise visitors. Wash your hands before handling and no visitors please. Your baby needs you as much as you need him/her.
